2019 Top Prior Authorization Solutions: PracticeSuite
It may be impossible to name any task more unpleasant than waiting on hold with an insurance carrier in an attempt to obtain preauthorization for a patient procedure, referral, or prescription medication.
And the only way the situation can be worsened is when after 30 minutes, you’re told that the particular coverage sought is handled by a third-party administrator, or TPA. So, you calmly ask for the contact information and start all over with new phone call.
In our prior authorization review of the best solutions for 2019, we’ve ranked seven vendors as the top options to help medical practices automate, cut cost, recover hours per day, and speed up authorizations for their patients.
Here, we provide an in-depth review of our number-one choice, AUTHORIZATION DESK by PracticeSuite.
Pros of AUTHORIZATION DESK
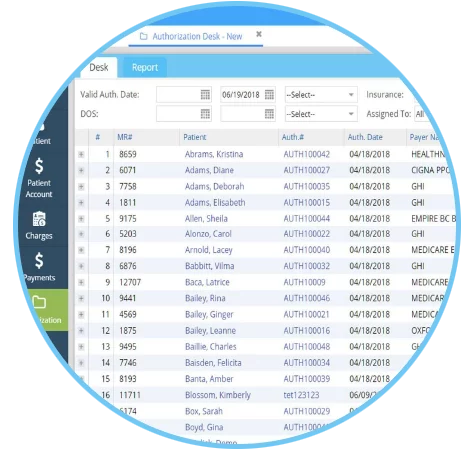
The first plus of PracticeSuite is great organization of the authorization workflow. Whether it’s an electronic approval request or a manual one, the software organizes your work queue into a coherent and comprehensible work flow. All authorizations are visible to the entire staff with a patient status of pending (review), complete, or denied. And once complete, the authorization details are connected to the patient file for future reference.
“Just being able to see all authorizations for the entire practice at-a-glance is a game changer” states Marie Serna, RCM Manager. “Status updates are another” she states. “We used to be in the dark until we called again and got an update”. “Now, if further documentation is required, we know it without having to pick up the phone”.
The ability to attach or fax documents without waiting on hold is yet another way the application saves time. The same applies to appealing denied approvals and retro-authorizations – all are easily managed within the application’s dashboard.
While not every carrier is able to receive documentation electronically, all of them receive faxes, so the e-fax feature of the application saves time here too. The patient’s Auth-Status can be updated manually in such cases to keep the other staff abreast of the pending status stage.
While some practices chose to keep authorizations in-house and use the software primarily to manage the process, others find it more beneficial to outsource the entire process to PracticeSuite’s Expert Services Team who are able to expedite prior authorizations from start to finish. The application triggers a notification whenever Payer Rules & CTP Codes match for a required prior authorization. The team then immediately goes to work to obtain the auth. The process takes hours instead of days, and days instead of weeks.
Plan adherence and patient satisfaction are key here. The longer the wait time, the greater risks there are of medication abandonment and care-plan failure. Fast action from the start ensures better clinical outcomes for patients. “We are extremely happy with the AUTHORIZATION DESK application” states Mrs Serna. “We’ve come to depend on it, and don’t want to think of living without it”.
Cons of PracticeSuite Prior Authorization Software
If there are any cons about the application, it would be for more payers to adopt electronic determination of benefits so that the process was streamlined for more plans and patient scenarios. The limitations are really on the part of the insurance carriers. But more are adopting EDI standards for electronic transactions.
In order for greater adoption to take place though, States have step up their game and apply the pressure. Nobody wants to wait on hold only for a benefits manager to tell them a service is denied for lack of medical necessity after a trained physician has just ordered a treatment or referral to a specialist.
Learn more about PracticeSuite’s PriorAuth Software.



