PracticeSuite for Pulmonology
Pulmonology EHR, Practice Management, and Medical Billing Software
Manage Your Entire Practice On A Single Platform. With an affordable all in one solution for in-office and remote patient care. PracticeSuite provides flexible workflows to help organize your practice and keep it operating at peak efficiency; as well as a complete end to end virtual practice that allows you to treat any patient, anywhere, on any device.
- Addiction Medicine
- Cardiology
- Dermatology
- Endocrinology
- Family Practice
- Gastroenterology
- Mental Health
- Nephrology
- Obstetrics Gynecology OBGYN
- Oncology
- Ophthalmology
- Orthopedics
- Otolaryngology ENT
- Pain Medicine
- Physical Therapy
- Pulmonology
- Plastic Surgery
- Podiatry
- Psychiatry
- Radiology
- Rheumatology
- Urology
Adaptive systems, intuitive workflows, and impactful patient care for pulmonologists
Improve efficiency with software that leads through the coding process
Optimize analysis and data integration from imaging devices
Support patient monitoring with a built-in EHR dashboard
Benchmark reimbursement rates with robust KPIs
Over 15,000 medical professionals from solo practitioners to large groups and medical centers rely on PracticeSuite’s cloud based medical billing technology to efficiently run their practice. Every feature required to run 150 different practice specialties is available but the system allows you to customize and simplify screens to see only what you want and need in each area of the software.
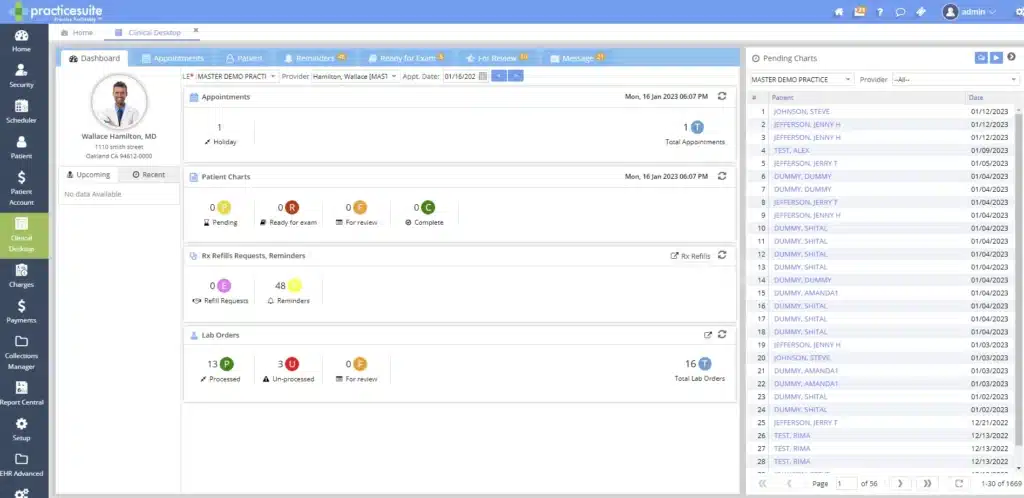
The PracticeSuite platform is designed to handle the specific complexities of pulmonology. Achieve high patient satisfaction, consistent revenue growth, and clearer documentation
See what Practice Management users are saying about PracticeSuite
“As a small business owner, it is a great way to store patient information, bill and be compliant. It is very simple to use!! Love being able to send bills out electronically. Every time I have contacted support, my issue was resolved immediately. Support is outstanding!!!”
– Dawn, Office Manager
“I am thoroughly satisfied with this product. Switching over to PracticeSuite has allowed me to bill my patients more efficiently and in turn made more money for my practice. My favorite feature by far is the outstanding support team. They are always there when you need them and they have assisted me with every problem I have encountered.”
– Matthew, Office Manager


